Beyond the Clinic: How Strategy Saves Lives
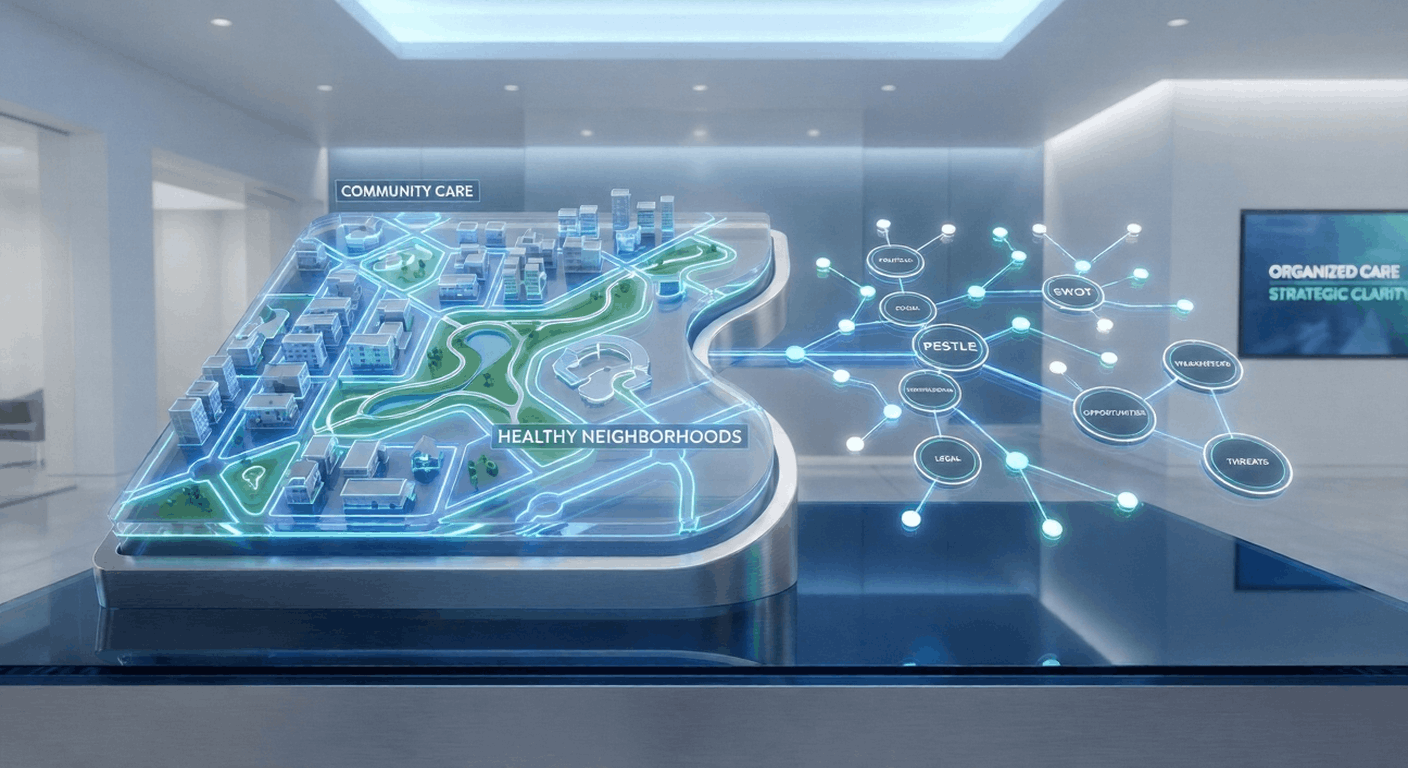
In health, the patient isn’t an individual sitting in an exam room; it’s an entire zip code. Developing effective community health strategies requires more than medical expertise; it requires a masterclass in organizational strategy.
Whether you are navigating a pandemic, tackling the opioid crisis, or addressing food insecurity, your success depends on how well you align disparate partners (hospitals, NGOs, and local government) around a single, cohesive plan. That’s where the Strategic Analysis Toolkit becomes your most valuable diagnostic tool.
Phase 1: Diagnosing the Environment
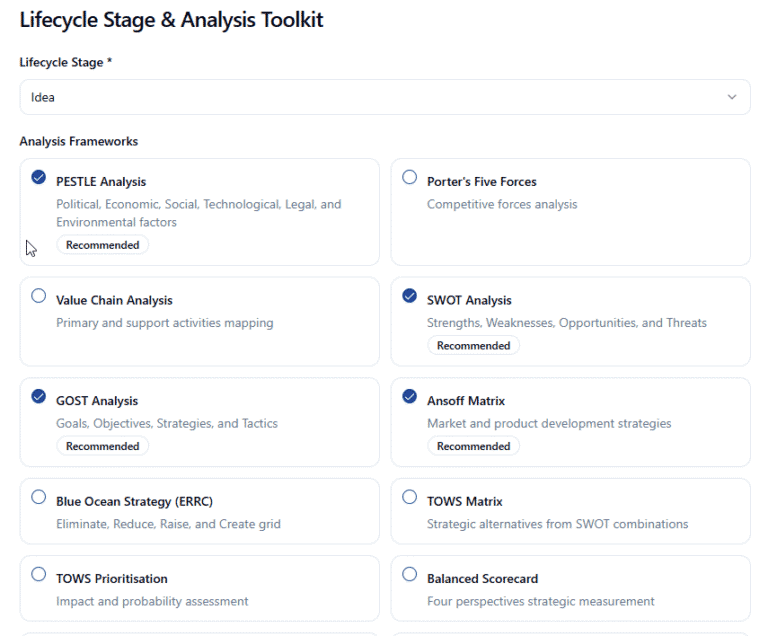
Before you can improve health, you must understand the environment that shapes it. We start with a PESTLE analysis. In population health, Political factors might include local funding shifts, while Social factors delve into the Social Determinants of Health (SDOH), such as education and housing.
Next, we examine Porter’s Five Forces. Who are the other players in your community? By understanding the bargaining power of insurers and the threat of service gaps, you can better position your healthcare collective. Finally, Value Chain Analysis shows exactly where value (or health outcomes) is being lost in the patient journey, from initial outreach to long-term follow-up.
Phase 2: Finding Your Blue Ocean in Public Health
Once the foundation is set, you need to decide where to play and how to win. A SWOT analysis is standard, but in this context it identifies your community’s Strengths (such as strong local leadership) and Threats (such as a rising uninsured population).
But how do you align twenty different organizations? You use the GOST framework (Goals, Objectives, Strategies, and Tactics). It turns a vague “let’s get healthier” into a concrete, measurable roadmap. To truly innovate, we look to the Ansoff Matrix to determine whether to offer existing services to new populations or develop entirely new health programs. If your community is struggling with overcrowded ERs, a Blue Ocean Strategy can help you create uncontested space through innovative urgent care models or mobile clinics that don’t just compete for patients but solve the problem entirely.
Phase 3: Turning Insight into Action
The most beautiful strategy is useless if it gathers dust on a shelf. This is where Implementation Planning becomes critical. We use the TOWS Matrix to bridge the gap between your SWOT results and action. With TOWS Prioritization, your board can decide which community health initiatives deserve immediate funding and which can wait.
To keep everyone accountable, the Balanced Scorecard is essential. In population health, we don’t just look at the bottom line. We look at:
- Health Outcomes (Clinical success)
- Stakeholder Satisfaction (Community trust)
- Operational Excellence (Program efficiency)
- Innovation/Learning (Staff training and new tech)
Phase 4: Making Change Stick
Health behavior is notoriously hard to change. Kotter’s 8-Step Plan for Change provides the psychological and organizational framework for building urgency and sustaining a new health initiative. You aren’t just launching a program; you’re changing a culture.
Because healthcare is rarely one-and-done, we employ the PDCA Cycle (Plan-Do-Check-Act). This ensures that if a nutrition program isn’t lowering BMI within six months, you have the data-driven agility to pivot. Finally, our Executive Summary and What-if Scenarios help health leaders prepare for the what-ifs, economic downturns, new viral strains, or funding cuts, ensuring your community remains resilient.
Your Strategy, Simplified
Population health is too important to leave to chance or to fragmented spreadsheets. You need a centralized, professional hub where these world-class frameworks reside.
The Strategic Analysis Toolkit offers every framework mentioned here in a streamlined, collaborative environment. Stop guessing and start leading.
Ready to transform your community’s health? Explore the Strategic Analysis Toolkit now.